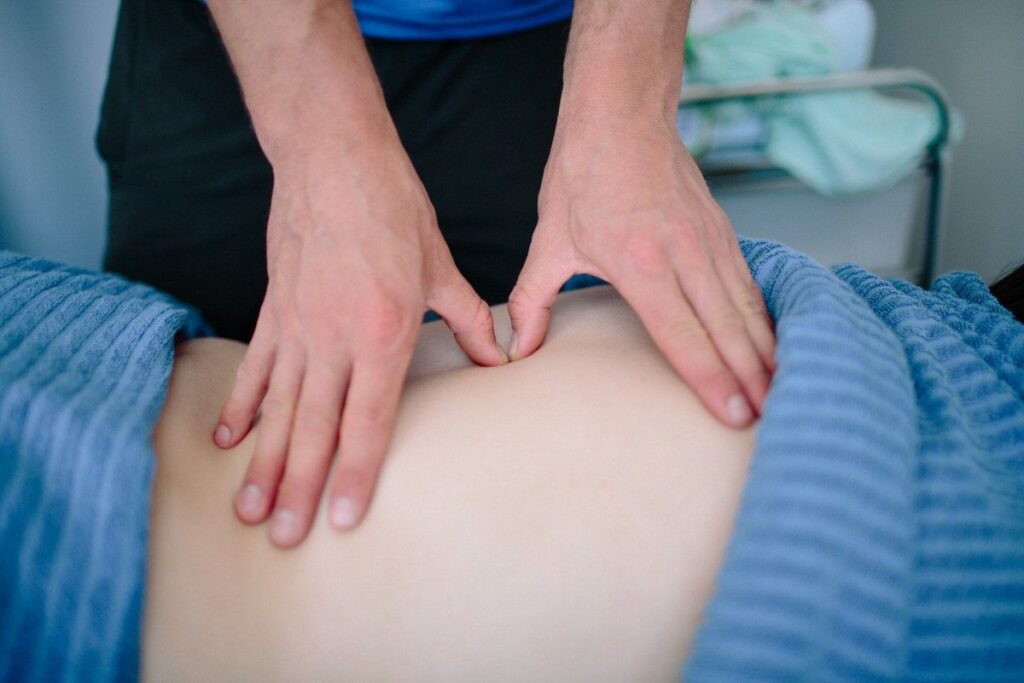
When it comes to manual therapy, two commonly used techniques in physiotherapy are mobilisations and manipulations. While they may sound similar — and are sometimes even used interchangeably — they are distinct methods with different applications, goals, and effects on the body. Understanding the difference between mobilisation and manipulation can help you feel more confident and informed during your treatment journey.
In this blog, we’ll explore how both techniques work, what they’re used for, and how your physiotherapist decides which approach is most appropriate for your condition.
What is Manual Therapy in Physiotherapy?
Manual therapy is a hands-on approach used by physiotherapists to assess, diagnose and treat musculoskeletal pain and dysfunction. It can include techniques such as soft tissue massage, joint mobilisation, joint manipulation, muscle energy techniques and stretching.
The goals of manual therapy are to:
-
Improve joint mobility
-
Reduce pain and inflammation
-
Restore functional movement
-
Enhance circulation
-
Aid tissue healing
Among these, mobilisation and manipulation are two specialised techniques focused primarily on improving joint function.
What is Mobilisation?
Mobilisation is a controlled, gentle movement technique applied to joints and soft tissues. It involves slow, repetitive movements performed within the joint’s normal range of motion. Mobilisations are usually graded based on their intensity and depth — from light, small-amplitude movements (Grade I) to stronger, deeper movements approaching the joint’s end range (Grade IV).
Mobilisations are commonly used to:
-
Improve joint flexibility and range of motion
-
Reduce stiffness after injury or surgery
-
Relieve mild to moderate pain
-
Restore function in conditions like osteoarthritis, frozen shoulder or postural dysfunction
Your physiotherapist may apply mobilisations using their hands or specialised tools, depending on the location and severity of your symptoms.
Because mobilisations are gentle and controlled, they’re often the technique of choice for:
-
Older adults
-
Individuals recovering from surgery
-
Patients with chronic conditions or acute inflammation
-
Those new to physiotherapy or nervous about manual treatment
What is Manipulation?
Manipulation, on the other hand, involves a quick, high-velocity thrust applied to a joint, usually at or near the end of its range of motion. You may hear an audible “click” or “pop” during the technique — this is often a natural release of gas bubbles within the joint and is completely normal.
Manipulation is used less frequently than mobilisation and is typically reserved for specific conditions when rapid results are needed. It can be effective in:
-
Releasing joint restrictions or “locked” joints
-
Reducing acute pain or muscle spasm
-
Restoring sudden loss of movement
-
Enhancing overall spinal alignment and posture
Manipulation is commonly associated with spinal physiotherapy, especially for the neck and lower back. It can provide immediate improvements in mobility and pain relief for suitable candidates.
Key Differences Between Mobilisation and Manipulation
| Aspect | Mobilisation | Manipulation |
|---|---|---|
| Speed | Slow, controlled movements | Fast, high-velocity thrust |
| Range | Performed within joint’s normal range | Performed at end of joint range |
| Force | Gradual, graded pressure | Quick, sudden force |
| Sound | Typically silent | May produce a “click” or “pop” |
| Use cases | Joint stiffness, chronic conditions, gradual recovery | Acute restrictions, spinal pain, sudden loss of movement |
| Patient experience | Generally more gentle and relaxing | May feel intense, but often followed by relief |
Are These Techniques Safe?
Yes — when performed by a qualified physiotherapist, both mobilisation and manipulation techniques are safe and effective. Before using either technique, your physio will carry out a detailed assessment to understand your condition, medical history, and treatment goals.
In Australia, physiotherapists are highly trained and regulated professionals. Many undergo additional postgraduate training to perform manipulations safely and appropriately. Informed consent is always obtained before applying manual techniques.
Which Technique is Right for Me?
The decision between mobilisation and manipulation depends on several factors:
-
The nature of your condition (acute vs chronic)
-
Your age and general health
-
How much pain or stiffness you’re experiencing
-
Your response to previous treatments
-
Your comfort level with manual therapy
Sometimes, your physiotherapist may start with gentle mobilisations and progress to manipulation as your body adapts. In other cases, a one-off manipulation might provide the immediate relief you need before moving into strength and rehabilitation exercises.
Final Thoughts
Both mobilisation and manipulation are valuable tools in the physiotherapy toolkit, each with unique benefits and applications. While mobilisation offers a gentle, gradual way to restore movement and reduce stiffness, manipulation can provide fast, effective relief when used appropriately.
Ultimately, your physiotherapist will tailor your treatment plan to suit your specific needs, ensuring safety, comfort and long-term recovery.
If you’re dealing with joint pain, restricted movement or muscle tightness, book an appointment with our experienced physiotherapy team. We’ll assess your condition and discuss the most effective manual therapy options for your recovery.
Need help managing pain or improving mobility? Contact us today to book your personalised physiotherapy consultation.

When diagnosed with cancer, the journey ahead can feel daunting. With the physical and emotional challenges that come with treatment, many people often wonder how they can maintain their strength and quality of life. One powerful tool that’s gaining recognition in cancer care is exercise. From maintaining muscle mass during chemotherapy to improving overall well-being, exercise has shown to provide significant benefits for cancer patients. Exercise physiology plays a key role in understanding these benefits and developing safe, effective exercise programs tailored to each individual’s needs.
Why is Exercise Important for Cancer Patients?
Cancer treatment, such as chemotherapy, radiotherapy, and surgery, can be physically taxing. Patients often experience fatigue, muscle wasting, weight loss, and a decrease in strength and endurance. These effects can have a significant impact on daily activities and overall quality of life. However, research shows that exercise can help mitigate these side effects, improving both physical and emotional health.
Exercise can be defined as any planned, structured, and repetitive physical activity that improves or maintains physical fitness. For cancer patients, regular exercise helps reduce the impact of cancer-related fatigue, boosts energy levels, strengthens the immune system, and supports the maintenance of muscle mass and bone density. Exercise physiology focuses on understanding the body’s response to physical activity, and this knowledge is crucial when designing exercise programs for cancer patients.
Maintaining Muscle Mass During Chemotherapy
One of the most concerning effects of chemotherapy is muscle wasting, also known as cancer cachexia. This condition leads to a significant loss of muscle mass and strength, which can worsen fatigue and limit mobility. Chemotherapy targets rapidly dividing cells, which include not only cancer cells but also healthy cells, such as those in muscles. As a result, patients often experience a loss of lean body mass, making it harder to perform everyday tasks.
Exercise, particularly resistance training, has been shown to be effective in countering muscle loss and promoting muscle retention during chemotherapy. Studies have found that engaging in strength-based exercises, such as lifting weights or using resistance bands, can stimulate muscle growth and prevent further deterioration. The key is to start at a manageable level and gradually increase intensity, ensuring that the body is not overstressed.
Exercise physiology plays an essential role in guiding cancer patients through this process. By designing a program that targets the muscles most affected by treatment, exercise physiologists ensure that patients are engaging in the right exercises in the right way to maintain muscle mass safely. Whether through resistance training, functional movement exercises, or even bodyweight exercises, staying active can help patients preserve their strength during treatment.
The Psychological Benefits of Exercise for Cancer Patients
Aside from the physical benefits, exercise also has a profound impact on mental health. A cancer diagnosis and the stress of treatment can lead to feelings of anxiety, depression, and isolation. Exercise has been shown to improve mood, reduce stress, and help manage symptoms of depression, which are common among cancer patients.
Endorphins, the body’s natural mood-boosting chemicals, are released during exercise, promoting a sense of well-being. Furthermore, the routine and sense of accomplishment associated with exercise can foster a sense of control, which is often lost during the cancer journey. These psychological benefits, in turn, can improve adherence to treatment and enhance overall quality of life.
Reducing the Risk of Cancer Recurrence
Research also suggests that regular exercise can help reduce the risk of cancer recurrence. Studies have shown that patients who engage in moderate physical activity after cancer treatment may experience a lower risk of their cancer returning, particularly in breast, colon, and prostate cancer survivors. Exercise can improve immune function, regulate hormones, and reduce inflammation—all factors that play a role in cancer progression.
While more research is needed to fully understand the mechanisms behind this relationship, the evidence so far is promising. For cancer survivors, staying active can be an important step in long-term health management.
Building a Safe and Effective Exercise Program
When it comes to exercise for cancer patients, safety is key. Every individual’s situation is unique, so it’s important to tailor exercise plans to the person’s specific needs, treatment stage, and fitness level. Exercise physiology plays a crucial role in this process, using scientific knowledge of how the body responds to exercise to create a personalised plan that ensures maximum benefit with minimal risk.
The following are some general guidelines for creating an exercise program for cancer patients:
- Start Slow: Begin with low-intensity exercises such as walking, light stretching, or gentle yoga. As strength improves, you can gradually increase the intensity and duration.
- Incorporate Strength Training: Resistance exercises help build muscle mass and counteract muscle loss due to chemotherapy. However, start with lighter weights or resistance bands, and progressively increase as the body adapts.
- Focus on Flexibility and Balance: Cancer treatments can impact flexibility and balance, so incorporating exercises like stretching and balance training can improve coordination and reduce the risk of falls.
- Stay Hydrated and Rested: It’s crucial to listen to your body. Stay hydrated, rest when needed, and ensure that your exercise program is balanced with recovery periods.
- Consult an Exercise Physiologist: Before beginning any exercise regimen, especially during or after cancer treatment, it’s important to consult with a qualified exercise physiologist. They can design a program tailored to your specific needs and ensure that you are exercising safely.
Conclusion
Exercise plays an essential role in managing the side effects of cancer treatment, improving overall physical and mental health, and supporting the maintenance of muscle mass during chemotherapy. Through the guidance of exercise physiology, cancer patients can enjoy a tailored program that helps them stay active and improve their quality of life. Whether you’re currently undergoing treatment or are a cancer survivor, integrating exercise into your routine can provide numerous benefits, supporting your journey towards better health and wellness.
If you or a loved one is going through cancer treatment, don’t hesitate to consult an exercise physiologist to create a plan that works for you. Your body will thank you for it. Read more HERE

